We include products in articles we think are useful for our readers. If you buy products or services through links on our website, we may earn a small commission.
Can You Be Fat and Healthy? Yes!

Can you think of anything more demonized than fat-both as a food, and as part of our bodies? It’s no wonder then, that many of us are asking “can you be fat and healthy?”
Entire industries of diet, exercise, and food production are built around the fallacy that fat is unhealthy, ugly, and unnatural.
The truth is, storing fat on our bodies and eating animal fats is healthy. In fact, it’s the most important evolutionary adaptation in human history. Without the ability to consume and store fat, the human species would have been snuffed out millennia ago.
From this perspective, obesity is not a disease. It’s an expression of our genetic inheritance. Studies show that between 20-75% of people who meet the criteria for obesity have no negative health markers.
For others who carry ‘excess’ fat along with negative health markers, obesity itself is not the cause of these problems, but a symptom of a larger problem–a standard American diet combined with a sedentary lifestyle.
In this article, we’ll explore how obesity is just one of the many symptoms of metabolic disorders caused by a diet high in carbs, industrial oils, and added sugars.
As you’ll see, focusing on losing weight to “get healthy” is misguided. The real key to metabolic health is changing what we eat.
Table of Contents
Why does the Body Store Fat?
The body stores fat as a key survival mechanism.
As our caveman ancestors learned how to scavenge and then hunt animal fats, they evolved a powerful metabolic relationship to this superior source of energy for our bodies, and especially our massive brains.
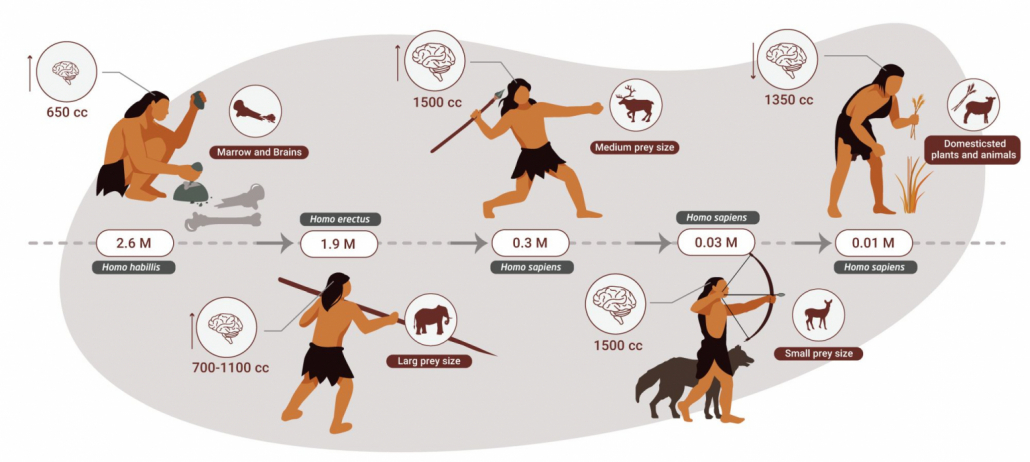
Humans are Designed to Store Fat as Energy
The ability to store fat on our bodies became an amazingly efficient way to supply our bodies and brains with energy, both during times of plenty and during leaner times.
We, modern humans, have inherited this genetic legacy in the following ways:
- We easily store fat on our bodies
- We easily metabolize fat into energy
- Our hunger hormones trigger us to eat more calories when we lose weight in an attempt to replenish our fat stores
These factors mean that when you gain a few pounds, your body experiences this as a major success, and it will fight hard to keep any extra weight.
Humans are Fat Animals
When compared to our primate ancestors, humans are extremely fat. For example, the leanest version of a human is a male bodybuilder. On average, a male bodybuilder still has 2-3 times more fat than other primates.

A lean 165lb (75kg) man stores over 100,000kcal of energy in fat. If we had to store this energy as carbs (like plants) we would weigh 40-60kg more because glycogen (the form of stored carbs in the human body) is less energy-dense than fat and is stored alongside water molecules.
40-60kg is the equivalent of carrying 2 packed suitcases. Imagine trying to hunt while lugging around this extra load.
Let’s turn next to human babies, who are notoriously fat. This is not the case for other primates, whose infants are very lean.
The fatness of babies at birth allows the body to turn that abundance of fat into fuel for the baby’s large and rapidly growing brain. Human babies even outdo baby seals when it comes to fatness. While chimps come in at only 3% fat.
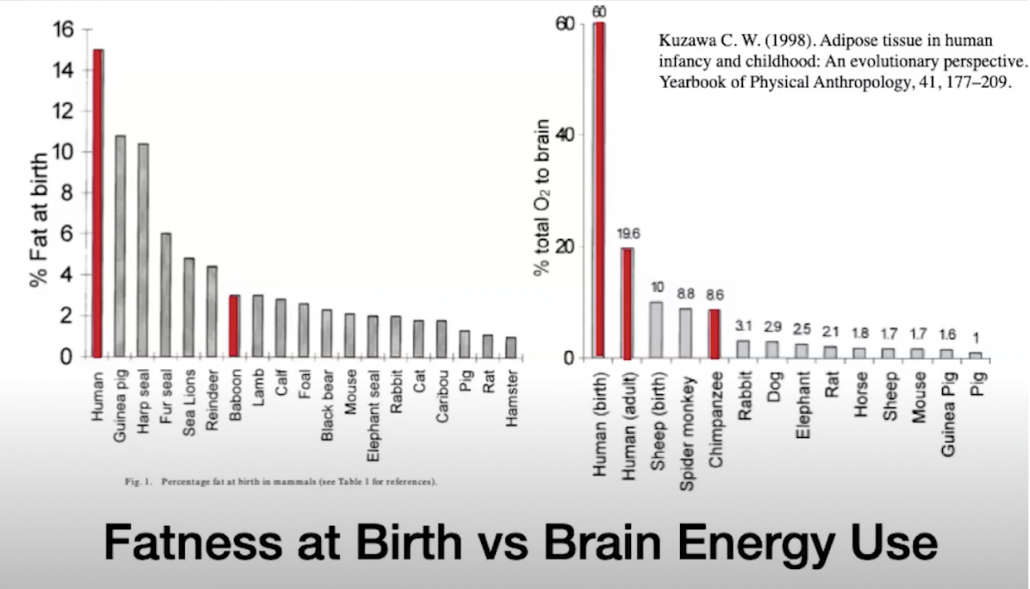
The human brain is 2.5 times as large as a chimpanzee brain. This echoes our fatness relative to chimps, again suggesting that fat is essential to the thing that makes us human–our massive brains. Our desire for and use of fat leads researchers like Amber O’Hearn to deem us “lipivores” or primarily fat eaters.
Why It’s So Hard to Lose Weight
When you dig a bit deeper into the importance of fat for both developing and adult humans, it makes sense that the body would do everything in its power to store and maintain body fat.
Since 1969, research has shown that losing only 3 percent of body weight results in a 17 percent slowdown in your metabolism.
When you lose weight your body thinks it’s being starved and responds automatically in two ways:
- Your body unleashes a powerful dose of hunger hormones, ghrelin and leptin
- Ghrelin causes you to crave high calorie, high-carbohydrate foods that make you as fat as possible as fast as possible
- At the same time, your leptin levels plummet. Leptin is the hormone that tells you when you feel full
- The combination of these hormonal forces and unlimited access to conventional high-carb diets are a recipe for boosting our fat stores
When we try to lose weight, there is a disproportionately large fall in circulating leptin in spite of only modest fat loss.
This fall in leptin triggers makes us feel hungry, compels us to seek “reward-related” behaviors, and can cause us to feel depressed which further motivates us to search for soothing through high-calorie foods.
Collectively, the nutritional, industrial food, and dietary establishments seem to be willfully ignorant of these processes–or in some cases to knowingly profit from them.
And, egregiously, we’re told to cut calories, especially when calories come in from the most satiating, hunger-suppressing food–fat from whole animal foods. As you’ll see, these recommendations are deadly wrong!
Being Fat and Being Healthy are Not Exclusive
Another important point that the medical and nutritional establishments have ignored is that body fat is not an accurate measure of health.
It is true that large-scale population studies find that, on average, fatter people have worse cardiovascular health than thin people. But people are not averages.
Numerous studies have found that between 30-75% of people classified as obese may be metabolically healthy.
Signs of Being Fat and Healthy
To be metabolically healthy obese (MHO) means 5:
- lower liver and visceral fat, but higher levels of subcutaneous leg fat
- greater cardiorespiratory fitness
- no signs of elevated blood pressure
- No insulin resistance
- Normal cholesterol
- Greater physical activity
- lower levels of inflammation
- normal adipose tissue function compared to people with metabolically unhealthy obesity
- Carrying fat around the thighs and but, but not the midsection
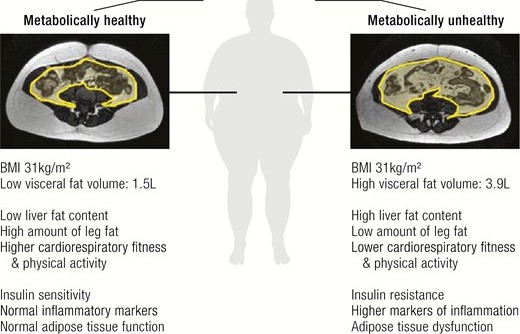
Skinny People Can be Metabolically Unhealthy
Just as many fat people can be healthy, lean and normal-weight people can be unhealthy.
Studies show that up to 30% of non-overweight people fall into the category of metabolically unhealthy lean people.
A 2016 study that followed participants for an average of 19 years found that metabolically unhealthy lean people were twice as likely to get diabetes as healthy fat people.
Indicators for unhealthy lean people include high levels of inflammatory markers, the prevalence of non-alcoholic fatty liver disease, and carrying fat around the mid-section, but not the thighs and butt.
If it’s Not Fat that is Killing Us, What is?
Science and nutrition journalist Michael Hobbs writes that the approach to obesity is “one of the largest gaps between science and practice in our own time. Years from now, we will look back in horror at the counterproductive ways we addressed the obesity epidemic and the barbaric ways we treated fat people—long after we knew there was a better path.”
The focus on demonizing fat, blaming obesity for our health issues, cutting calories, and eliminating meat and animal fats is completely backward. You can be fat and healthy, and eat fat to get healthy.
Our cultural and institutional obsession with body weight is a collective gaslighting. It conveniently turns our attention away from what is really killing us– a high-carb diet of processed junk combined with a sedentary lifestyle.
It’s not how much we’re eating, but what we’re eating that matters.
And it’s not always how fat we are that matters, but the unhealthy food and lifestyle choices that make us metabolically sick. Extra weight is only a symptom but not the cause.
We know that diet is the leading cause of death in America, responsible for more than five times the combined fatalities from gun violence and car accidents.
We know that 60 percent of the calories we eat come from processed foods that are high in sugar, grains, and vegetable oils.
We know that these “plant-based” foods at the core of the Standard American Diet, are the root cause of the “diseases of civilization” including :
- heart disease
- hypertension
- type 2 diabetes
- epithelial cell cancers
- inflammatory diseases (including autoimmune diseases, bowel disorders, osteoporosis, infertility, and more)
These are called ‘the diseases of civilization’ because they are virtually non-existent in traditional societies that eat a whole foods diet based around animal products.3 [10]
Each of these diseases has metabolic disorders and chronic inflammation at its root, not obesity.
What Happens When Obese People Cut Carbs and Eat More Fat?
Let’s take a look at recent controlled trials showing us what happens when we cut out carbs and eat more fat.
The Effect of Spanish Ketogenic Mediterranean Diet on Nonalcoholic fatty liver disease– Perez-Guisado and Munoz-Serrano

In this controlled feeding trial of the Spanish Keto Mediterranean Diet (SKMD), researchers dramatically cut carbs and boosted fats, but didn’t cut calories.
The participants included 22 obese men with metabolic syndrome.
After 12 weeks researchers found that for all 22 participants :
- Fasting blood sugar levels dropped from a pre-diabetic 118 to an ideal 91
- Subjects lost an average of at least 30 pounds
- All participants no longer had metabolic syndrome
- They lost an average of 6 inches (16 centimeters) from their waist
- Body mass index (BMI) dropped from 37 to 31.5: This represents a change from class 2 obesity to the low end of class 1
- An increase in “good” HDL cholesterol from 44 to 58
- A decrease in triglycerides from 224 to 109
- A change from “prehypertensive” to “normotensive”
- Markers for fatty liver disease including liver enzymes and liver fat reduced, and in some cases completely resolved
It is important to highlight that most participants were still on the lower scale of obesity after 12 weeks. Yet their metabolic syndrome was completely resolved.
This tells us that it wasn’t being fat, and then losing weight that cured the metabolic disease. Rather, these dramatic metabolic changes can be attributed to the power of dietary change itself. They also show that it’s entirely possible to be fat and healthy.
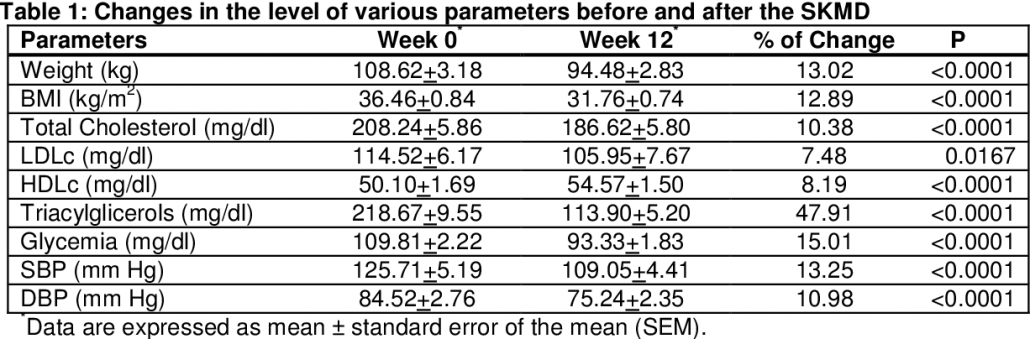
This power of low-carb high-fat diet to make us metabolically healthy even while still obese is reflected in numerous other studies.
Comparison of low- and high- carbohydrate diets for type 2 diabetes– Tay et al.

In this 2015 study looking at 115 obese people found that when comparing low-carb, high-fat diet with a high-carb diet, participants on the LCHF diet showed greater blood sugar control and significant reductions in the use of diabetes medications.
Effect of low-calorie versus low-carbohydrate ketogenic diet in type 2 diabetes- Hussain et al.

This study looked at 363 overweight and obese people, 102 of which had type 2 diabetes. Researchers found that a very low-carb, high-fat ketogenic diet resulted in significant blood sugar control and medication use reduction. Some participants discontinued use of their medications altogether.
Effects of a HFLC diet compared to a low-fat high carbohydrate (LFHC) diet on the change in weight loss, cardiovascular risk factors and inflammation in subjects with obesity– Ruth et al.

This 2014 study compared the effects of a high-fat low-carb diet with a low-fat high carb diet on 55 obese adults for 12 weeks.
Researchers found that the HFLC diet was superior at reducing triglycerides and improving HDL cholesterol while reducing levels of the inflammation marker C-reactive protein .
Interestingly, both diets promoted similar changes in body weight and composition. Again we see that it’s not how fat we are that matters most. Metabolic health has much more to do with what we are feeding ourselves.
Key Diet and Lifestyle Factors Making us Sick
To better understand the powerful metabolic benefits of HFLC eating, let’s now consider what a high-fat low-carb diet eliminates.
Vegetable Oils
Numerous randomized control trials using humans and animals, historical evidence, and large-scale observational studies show us that our consumption of vegetable oils is one of the greatest dietary blunders in human history.
Vegetable oil has been shown to cause inflammation and disrupt hormone signaling in ways that lead to increased risk of :
- Cancer
- All-cause mortality
- Heart disease
- Depression
- Neurodegenerative disorders including Alzheimer’s, dementia, and Parkinson’s disease
- Impaired fertility
- Obesity
Though there are many factors in modern life that contribute to the rise of inflammatory diseases that kill the most people across the globe, only heavy smoking is more deadly than vegetable oil consumption.
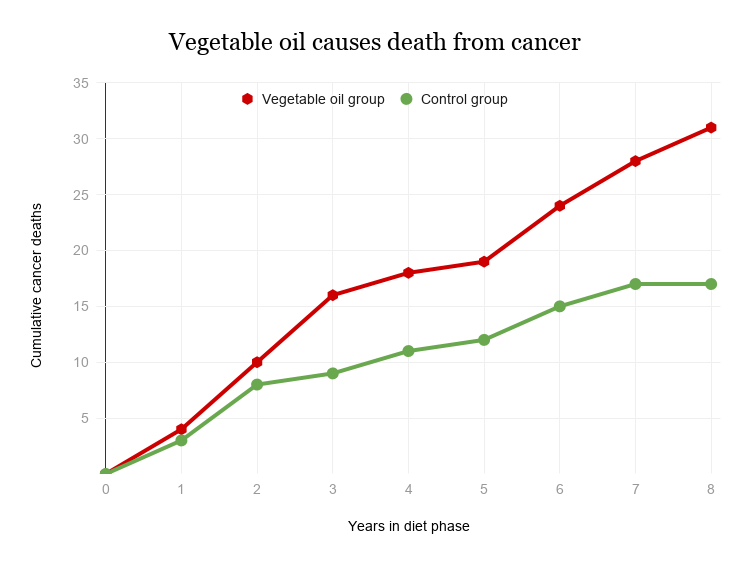
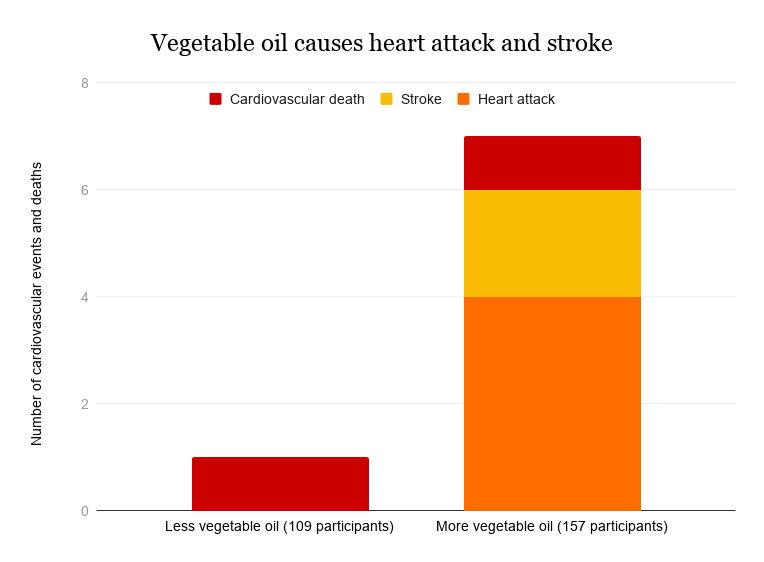
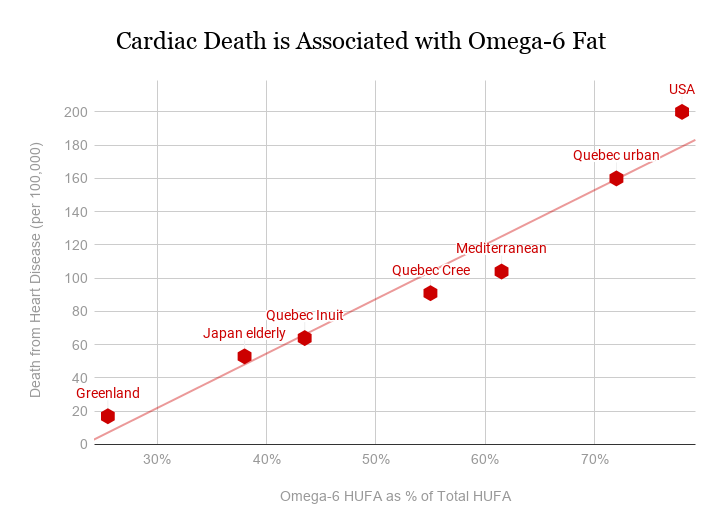
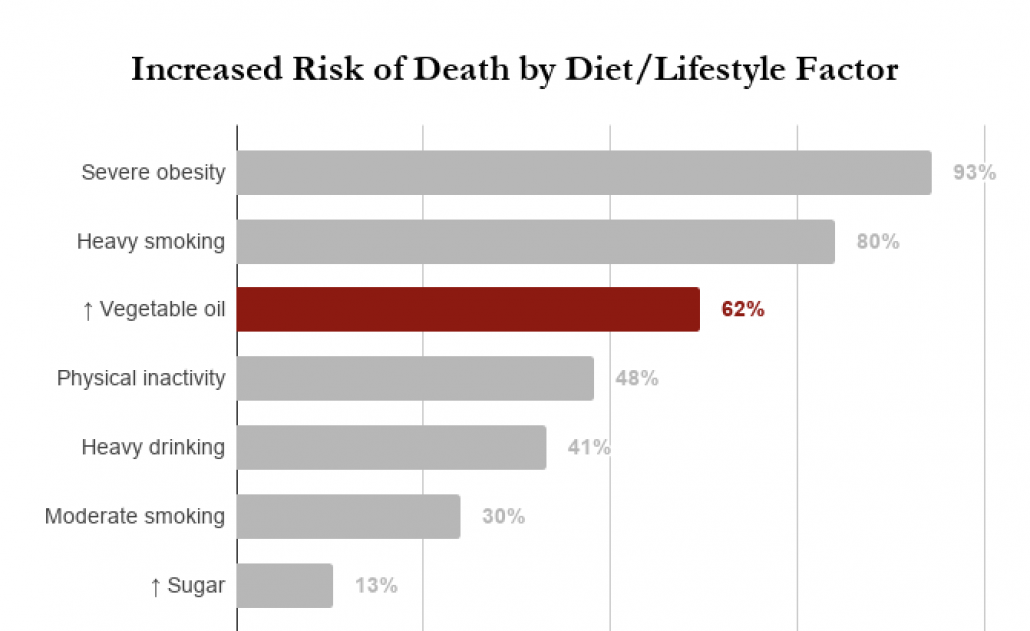
Read more about why vegetable oil is bad for you here.
Added Sugars
The average American gets between 50%-60% of their calories from carbohydrates and 16% from added sugars alone.
Sugar intake has been shown to be responsible for many of the problems associated with obesity including increased inflammation, higher triglycerides, higher, blood pressure.
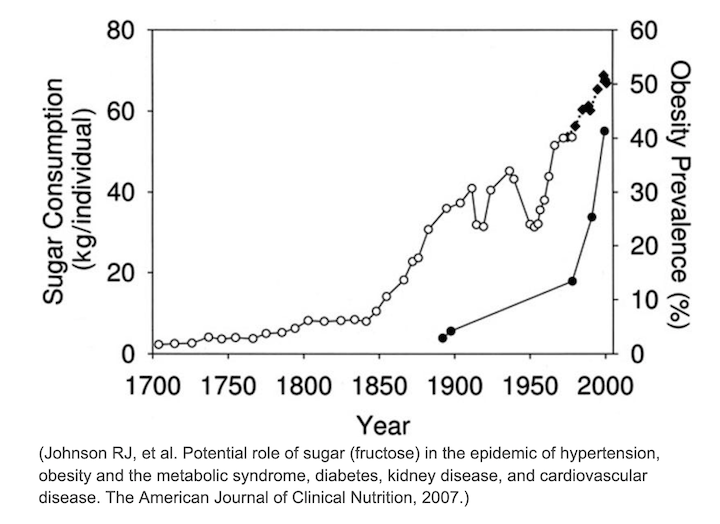
Other research has shown that consuming sugar promotes the metabolic disorder that underly obesity.
Our chronically high level of sugar intake factors in numerous metabolic diseases and disorders including diabetes, heart disease, cancer, infertility, and various autoimmune and neurodegenerative diseases.
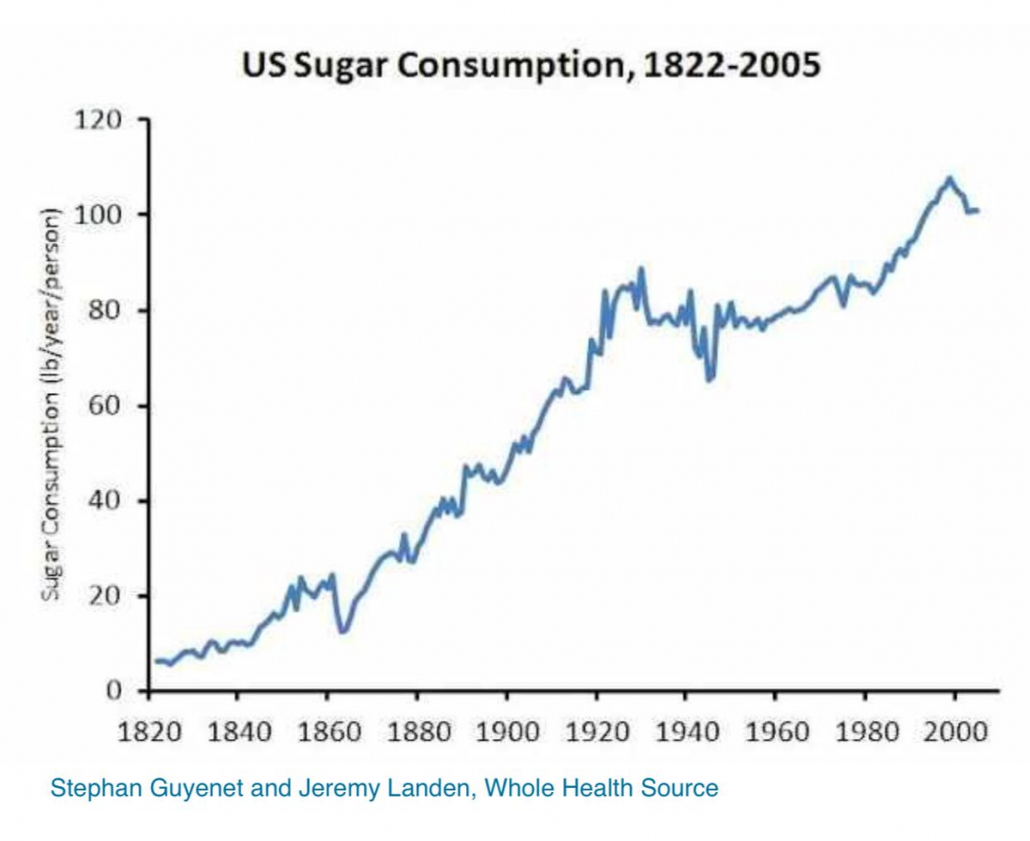
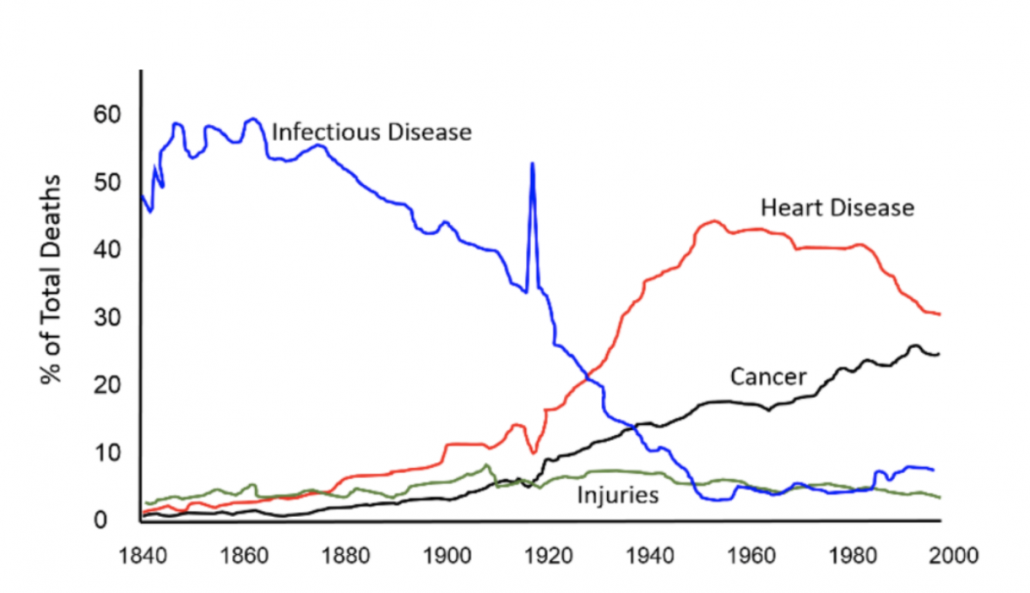
Learn more about the dangers of sugar here.
Lifestyle Factors
Our food systems and dietary guidelines are part of larger unhealthy lifestyle trends.
Stress and Anxiety
With the 24-hour news cycle, and our place within the social media attention economy, anxiety disorders have become the most common mental illness in the U.S., affecting around 40 million adults — almost 1 in 5 people.
When we’re stressed, our bodies secrete the stress hormone cortisol and the hunger hormone ghrelin. Cortisol increases appetite and motivation to eat, while ghrelin increases appetite and reduces depressive feelings.
In the context of hunter gatherer lifestyle, this makes sense–our greatest stress was finding calories. It would motivate us to go and hunt fatty animals. But in our modern society it these hormones motivate us to get calories from the most accessible, calorie-rich, and palatable source–sugary processed junk foods.
Long Commutes and Access to Fast Food
Americans are traveling further by car–thanks to urban sprawl. Between 2005-1016 workers commuting more than 90 minutes each way grew by more than 15 percent. 6 This means we’re walking less, and have less time to prepare food and move our bodies.
This increases reliance on prepared foods high in carbs and seed oils, while prohibiting us from doing physical activities that reduce stress.
Long commutes also promote the consumption of fast food. And nearly 20% of all American meals are consumed in the car.
At least 1 in 4 people eat fast food on a daily basis. [7] And Americans consume 31% more packaged food than fresh food.
Studies show that consuming processed foods contributes to numerous diseases and disorders, including diabetes, heart disease, infertility, cancers, and autoimmune diseases.
The Medical Establishment
There are numerous problems with the medical institution that harm our metabolic health. These problems begin with most doctors’ ignorance of the importance of nutrition–especially high-fat low-carb eating.
This problem begins in medical school. According to a 2015 survey, med students receive an average of only 19 hours of nutrition education over four years of schooling. This is down five hours since 2006.
A study from 2012 recorded 461 interactions between patients and doctors. It found that only 13 percent of patients were given a plan for diet or exercise. And only 5 percent got help to arrange a follow-up visit. The problem is doctors just don’t feel like they have the time.
These egregious shortcomings when it comes to diet and lifestyle support make sense within our system. Primary care physicians only get 15 minutes to meet with patients per appointment. While pokes, pricks, and procedures like CT scans and blood tests get much higher insurance reimbursements than diet and nutrition counseling.
Reclaim Your Metabolic Health with Dr. Kiltz’s 3 Pillars
Dr. Kiltz has created three pillars of health and wellness that will help you reclaim your metabolic health.
Rather than targeting fat as something your need to lose, Dr. Kiltz’s approach calls for eating more fat, cutting carbs, intermittent fasting, practicing low-impact movement, and destressing through meditative and creative practices.
Here’s a brief introduction to each pillar.
HFLC Eating
High-fat low-carb eating means dramatically reducing carbs. This means substituting grains, pasta, bread, rice, legumes with fatty whole foods like:
There are many variations of high-fat low-carb ways of eating with carb intake ranging from 0-100 grams per day. Some of the most popular examples of HFLC eating are:
Intermittent Feasting (Fasting)
For the hundreds of thousands of years when our ancestors had to feast on successful hunts while the meat was fresh. Then they fasted between successful hunts.
Intermittent fasting research show that mimicking this ancestral fasting/feating eating pattern can offer numerous health benefits including :
- Restoring gut health
- Blood sugar regulation
- cholesterol and triglycerides control
- Supports heart health
- increased lean muscle mass
- Stimulates human growth hormone
- Stem cell production
- supports mindful eating habits
Research suggests that our brains are hard-wired to function optimally during times of food scarcity and that our cognitive ability diminishes when we don’t fast [6].
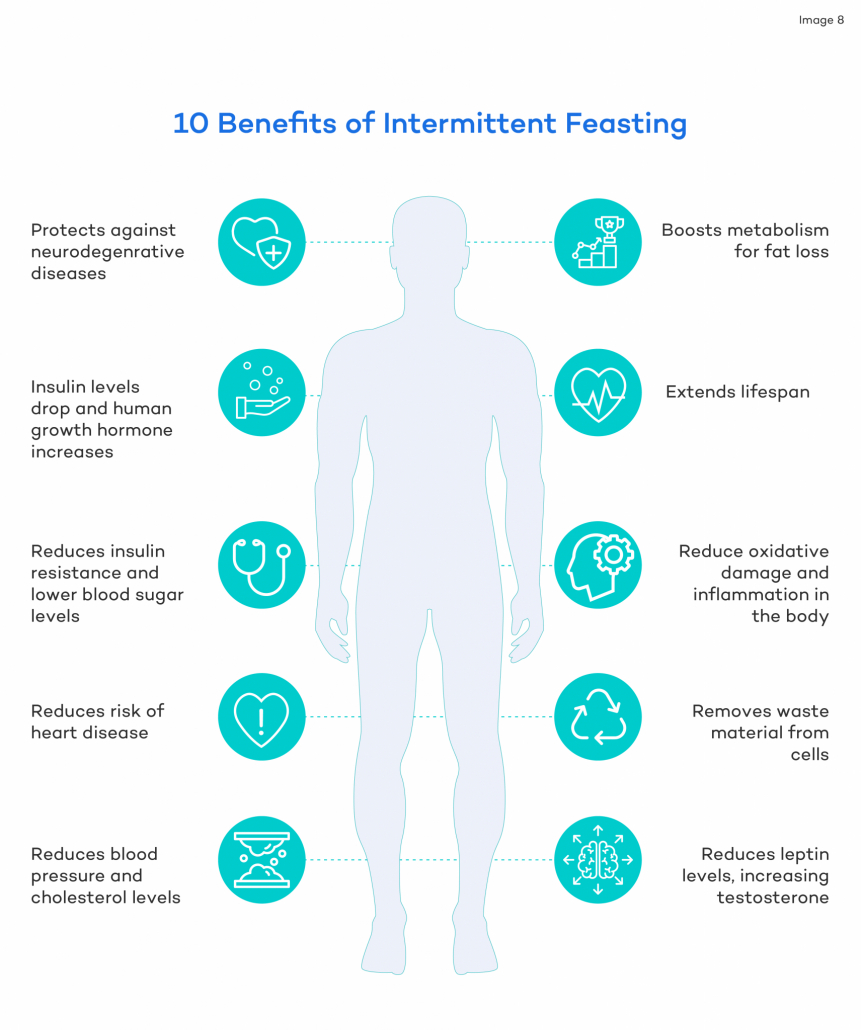
Low-Impact Movement and Plenty of Rest
Our hunter gatherer ancestors rested as much as possible. And its safe to say, they weren’t intentionally wearing out their bodies with CrossFit.
Our ancestors’ main source of exercise was walking around 10km a day, interspersed with some brief periods of running after prey.
You can bring low-impact restorative movement into your modern life by:
Rest
As important as movement is rest. Rest periods give our bodies time to digest, heal, and release nervous system activation we’ve accumulated during our busy lives.
And you can bring restoration to your mind and emotional body by doing:
- Gratitude practices
- Meditation
- Positive thinking
- Positive affirmations
- Mindful eating
- Enjoyable hobbies like pottery, painting, fishing
You can learn more about Dr. Kiltz’s three pillars to optimal health and wellness here.
Having more body fat is not a disease. At worst it’s a symptom of deeper metabolic disorders caused by a diet high in carbs, seed (vegetable) oils, added sugars, and processed foods.
It is common to be fat, “obese”, and metabolically healthy, and it is also common to be metabolically unhealthy and lean or “normal” weight.
Our cultural demonization and fixation on dietary and body fat distract us from the root cause of chronic inflammatory diseases like cancer, heart disease, type-2 diabetes.
The fact is that humans are designed to thrive on fatty whole foods from animal sources and to store fat on our bodies that we can unlock for energy whenever we need.
Demonizing and cutting fat out of our diets, and shaming body fat disregards the dietary and physiological traits that helped our ancestors survive, and that made us human.




















