We include products in articles we think are useful for our readers. If you buy products or services through links on our website, we may earn a small commission.
The Latest Intermittent Fasting Research: What the Studies Tell Us

Intermittent fasting is one of the most explosive dietary trends in recent history. And thanks to its popularity, intermittent fasting research studies are on the rise.
Over the last few years, millions of people have taken up various intermittent fasting methods and report numerous powerful benefits.
As one of the most researched dietary techniques, science is revealing just what these benefits are, and how they come about.
Study after study is showing that intermittent fasting can reduce inflammation, accelerate weight loss, improve brain function, and promote cellular regeneration. [1]
Yet, because IF is still so new, even people who have reaped its rewards have questions about IF’s long-term safety and effectiveness.
In this article we’ll explore the highest quality and most up-to-date intermittent fasting research, and what it reveals about the pros, cons, and unknowns of this dietary routine.
Table of Contents
The Research on How Intermittent Fasting Works
Intermittent fasting research shows us that it’s effects can be attributed to 3 key factors:
- IF triggers a metabolic ‘switch’ towards fat burning
- IF helps people avoid junk food, eliminates most snacking, and supports more mindful eating practices.
- IF activates beneficial hormonal changes
The Metabolic ‘Switch’ From Sugar to Fat Burning
Intermittent fasting can trigger a drastic transition from carb-burning towards fat-burning, as if a metabolic switch has been flipped.
A 2020 review of numerous studies looking at the effects of intermittent fasting on heart health, stated, “this change from using glucose as energy to using fatty acids and ketones for energy is called intermittent metabolic switching.”3
And a 2019 scientific review of fasting’s benefits in the New England Journal of Medicine, further described this switching:
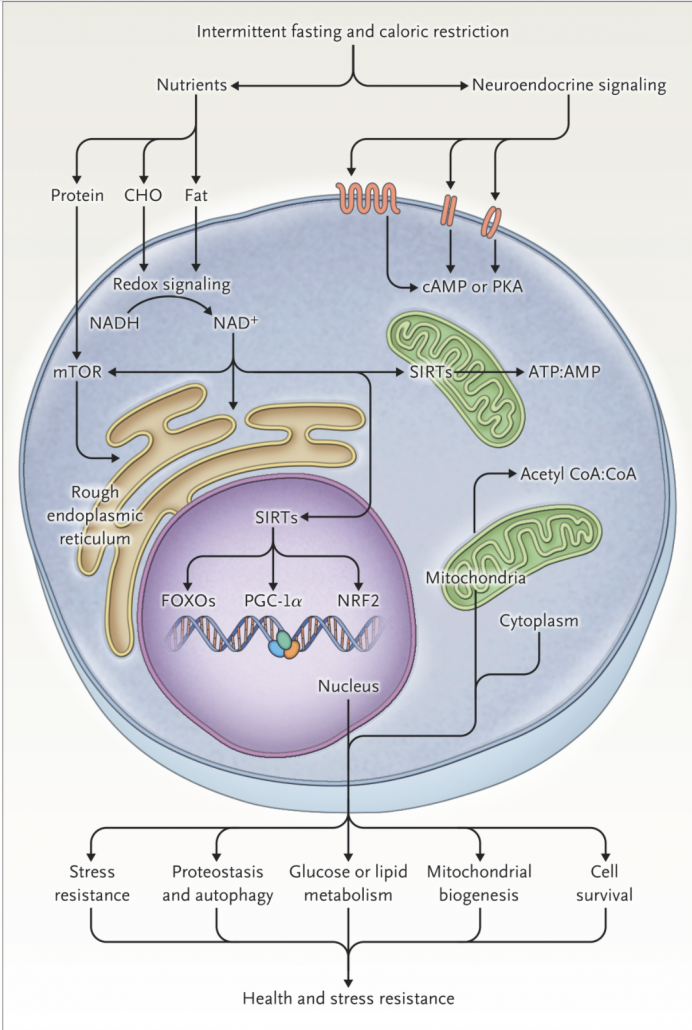
“Glucose and fatty acids are the main sources of energy for cells. After meals, glucose is used for energy, and fat is stored in adipose tissue as triglycerides. During periods of fasting, triglycerides are broken down to fatty acids and glycerol, which are used for energy.” [2]
Over time the body starts producing an even more efficient fat-based fuel source: the ketone.
“The liver converts fatty acids to ketone bodies, which provide a major source of energy for many tissues, especially the brain, during fasting. In the fed state, blood levels of ketone bodies are low, and in humans, they rise within 8 to 12 hours after the onset of fasting […] The timing of this response gives some indication of the appropriate periods for fasting in intermittent-fasting regimens.”
In other words, just 8-12 hours without food is enough to trigger ketone production and provide access to the numerous health benefits of ketosis. Going without food also makes your metabolism more efficient:
“The metabolic switch from the use of glucose as a fuel source to the use of fatty acids and ketone bodies results in a reduced respiratory-exchange ratio (the ratio of carbon dioxide produced to oxygen consumed), indicating the greater metabolic flexibility and efficiency of energy production from fatty acids and ketone bodies.”
Many studies show that intermittent fasting’s major benefits are independent of its ability to cause weight loss — they come from this metabolic shift.
These benefits include improved insulin sensitivity, blood pressure, cardiac function, muscular endurance, and more. [3]
Eating nothing > Eating junk
Intermittent fasting research tells us that the benefits of intermittent fasting can’t be fully attributed to ketosis. Nor can they be chalked up to calorie restriction, which some research implies becomes less helpful in the long run. [4][5]
In fact many of IF’s benefits might come from something far more obvious: abstaining from junk food.
Many of the animal studies that are used to support the efficacy of calorie restriction feed the control groups high-sugar, high-PUFA junk food. This choice of food essentially predetermined the outcomes. We don’t need an animal study to tell us that eating nothing is healthier than consuming processed fats and sugar.
One of the rare studies that fed their control group a healthier diet containing less sucrose and more antioxidants found no benefit to calorie restriction.
In other words, the benefits of calorie restriction — formerly thought to be a major factor in the health outcomes of intermittent fasting — may have been totally misattributed.
Besides, the metabolic shift caused by calorie restriction may be easily duplicated by eating a diet rich in healthy fats and balanced in amino acids.
Examples of this are found in various low carb diets, like carnivore, or mediterranean keto. And foods like bone broth and organ meats. These foods keep cells hydrophobic and ‘relaxed,’ two qualities that virtually ensure longevity.
That doesn’t mean intermittent fasting isn’t effective — if anything, it tells us that IF becomes even more effective when combined with a nose-to-tail diet that replaces junk food with superfoods that promote youth-related processes like a healthy glycocalyx, and reduced glycation.
Research-Backed Intermittent Fasting Benefits
Now that we’ve looked at why intermittent fasting works, let’s explore what intermittent fasting studies say about its top benefits. These include:
- Hormone optimization
- Improved body composition
- Increased insulin sensitivity
- Reduced inflammation
- Improved heart health
- Improved mindfulness
Hormone Optimization
Your body’s hormones, like its metabolic state, shift when you’re not eating. Storage hormones like insulin go down, while hunger hormones like ghrelin go up. [7] But that’s only the tip of the iceberg. Other powerful hormonal changes include:
- Human growth hormone levels rise, often dramatically. This increases fat burning, facilitates muscle gain, and reduces water retention. [8][9]
- Cortisol levels rise, then fall to below baseline. Cortisol is a stress hormone whose transient rise helps your body adapt to the intermittent fast. [10]
- Testosterone levels fall, then begin to rise. This shift further enhances fat burning while helping retain lean muscle tissue. [11]
Many of IF’s central benefits are a direct result of these hormonal shifts and the way that they affect cellular function and genetic expression. [12]
Improved Body Composition
Weight loss is one of the primary reasons people begin an intermittent fasting routine.
Intermittent fasting research shows that indeed IF is effective for weight loss.
A comprehensive 2020 study reviewing all 27 clinical trials to date found, “weight loss of 0.8% to 13.0% of baseline weight with no serious adverse events. Twelve studies comparing IF to calorie restriction found equivalent results. The 5 studies that included patients with type 2 diabetes documented improved glycemic control.”12
Though IF is not an explicitly calorie-restricting dietary practice, less frequent meals generally results in consuming fewer calories.
But as we discussed above, the effects of IF, including weight loss, have to do with hormonal shifts that speed up your metabolic rate.
Intermittent fasting ability to stimulate HGH and norepinephrine allows your body to access its fat stores with ease — so much so that studies show that short-term fasting increases your metabolic rate. [13]
One 2014 study looking at alternate day fasting found that adherents lost 3-8% of their body weight within 24 weeks–an unusually significant amount. [14]
This study’s participants also lost 4-7% off their waste circumference, meaning that they lost significant amounts of the harmful visceral fat. [15]
Perhaps even more impressive than potential weight loss is IF’s ability to ensure that these losses come from the right places i.e. fat, not muscle.
A 2011 review of the literature found that IF caused less muscle loss than more standard isocaloric diets. [16]
All in all, intermittent fasting research confirms that IF is a safe and effective tool for people who want to reshape their bodies.
Increased Insulin Sensitivity
Insulin resistance is a modern-day epidemic. Full-blown insulin resistance is known as type 2 diabetes, but even subclinical insulin resistance can cause high blood sugar, chronic inflammation. 2
Insulin resistance is largely attributable to eating a high-sugar, high-PUFA diet — the two substances that make up a huge portion of the calories in a Standard American Diet. [17]
Intermittent fasting may be a effective antidote. Studies show that IF has strong insulin-sensitizing effects. In turn, these lead to less blood sugar and a reduced risk of diabetes. [18]
Human studies show that several months of intermittent fasting can reduce blood sugar by 3-6% — and reduce baseline insulin levels by a whopping 20–31%. [19]
Less insulin means less fat storage, and reduced likelihood of prolific diseases like heart diseases and PCOS.
In animal studies, intermittent fasting is so effective for improving insulin sensitivity that it’s been shown to protect lab mice from diabetic retinopathy, a serious condition that can lead to blindness. [20]
It’s worth noting that this IF benefit may vary depending on your gender.
A 2005 study showed that women’s blood sugar regulation got worse, not better, after a 22-day regime of “alternate day fasting”. The stress hormone cortisol may be to blame. [21]
However, alternate day fasting is one of the most extreme intermittent fasting interventions. Other approaches like the popular 16/8 method, and circadian rhythm method are gentler and may be more effective for women.
You can learn more about intermittent fasting strategies for women here.
Reduced inflammation
Chronic inflammation is thought to drive the development of virtually all chronic diseases, even those like cancer that are often attributed to ‘genetic’ causes.
Inflammation Fast Facts
- Inflammation is an important tool that our bodies use to fight infections, but the excess inflammation-causing cells in modern humans may be a product of overeating.
- According to the World Health Organization (WHO) diseases related to chronic inflammation are the most significant cause of death in the world. [4]
- Researchers forecast that inflammatory diseases will only increase over the next 30 years, and in large part due to our modern eating habits. 5
- A 2014 study by the Rand Corporation estimated that Americans with at least one chronic inflammatory condition make up 60% of the population., While 42% has more than 1, and 12% of adults have 5 or more chronic inflammatory conditions. 2
- On a global scale, chronic inflammatory diseases kill 3 out of 5 people. These diseases include stroke, respiratory diseases, heart disorders, cancer, obesity, and diabetes. [5] [6] [7]
- Inflammation is usually caused by reactive oxygen species, including free radicals, that can react in damaging ways with your DNA.
Intermittent fasting provides a holistic solution for reduced inflammation by reducing the root causes of oxidative stress, including chronically elevated blood sugar levels.
The largest population studies exploring the effects of intermittent fasting on inflammation looked at Muslim’s during Ramadan, a holy month that calls for fasting during daylight hours. 3
A 2010 study found that fasting during Ramadan indeed limits inflammation 2. And researchers from a separate 2012 study found that Ramadan fasting, “attenuates inflammatory status of the body by suppressing proinflammatory cytokine expression and decreasing body fat and circulating levels of leukocytes.” 4
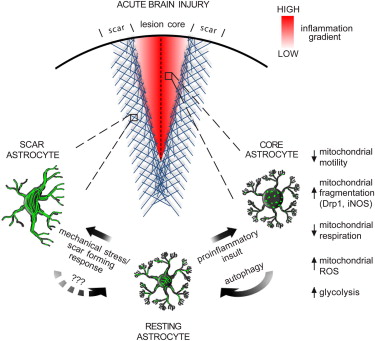
Similarly, a 2013 animal study found that fasting for more than 24 hours may lower inflammation by reducing oxidative stress levels in cells. In this brutal study, researchers injected the brains of mice with rabies, and looked at the effects of intermittent fasting on inflammation related specifically to these brain injuries.
They found that a key factor in the protective effects of IF was the activation of autophagy–controlled cell death, that actually benefited the health of other cells by improving mitochondrial (energy factories within cells) function.5
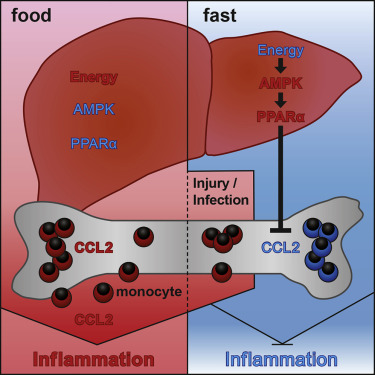
A 2019 study published in Cell, came to a similar conclusion that intermittent fasting reduced cells that cause inflammation called monocytes.
Interestingly, the monocytes that were present in the blood were less inflammatory for people and mice who were intermittent fasting, than for those who weren’t.5
Speaking to Healthline about the study, lead researcher Dr. Miriam Merad said, “Especially in the Western world, people eat all the time and that’s a fairly recent habit in human evolution…Somehow we have acquired dietary habits that are putting us at risk for inflammation.”6
One of these dietary habits may be the overabundance of plant foods that contain numerous naturally occurring plant toxins and antinutrients.
Improved Heart Health
Worldwide, heart disease is the leading cause of preventable deaths. [23] The good news is that intermittent fasting may improve several key risk factors for heart disease, including:
- Triglycerides
- Blood pressure
- Blood sugar levels
- Inflammatory markers
- LDL cholesterol (‘bad’ cholesterol) LINK
Much of the intermittent fasting research centered on heart disease comes from animal studies. However, the findings in previous IF animal studies have been found true for humans in later studies, which bodes well for the heart disease studies. [24]
Studies suggest that the heart-healthy effects of intermittent fasting are due in part to a number of factors including:
- Autophagy (cellular renewal)
- Ketosis
- Weight loss
- Reduced oxidative stress
- Eating in alignment with our internal circadian rhythm
A 2020 review of all that looked at the above factors in all the available literature on the use of intermittent fasting for heart disease concluded that: “Intermittent fasting appears to positively impact multiple cardiovascular risk factors including obesity, hypertension, dyslipidemia, and diabetes. Furthermore, intermittent fasting has been associated with improved outcome after a cardiac event.” 25
Since we’ve looked at the intermittent fasting research on ketosis, weight-loss, and oxidative stress (inflammation), let’s turn now to autophagy.
Autophagy
Autophagy, which literally means “self-eating,” can be a beneficial cellular process where old cells get recycled and renewed. Misshapen cells that might otherwise become fibrotic or even cancerous get removed. Think of autophagy as cellular spring cleaning!
The average person eating 3 meals a day with snacks in between dramatically limits autophagy — but the average intermittent fasting practitioner gives autophagy a powerful boost. [25]
A 2018 study found “the evidence overwhelmingly suggesting that autophagy is induced in a wide variety of tissues and organs (including the heart) in response to food deprivation.” 25
The role of autophagy in the heart is extremely complex in situtions of normal stress, and induced caloric stress from intermittent fasting. Though studies are still preliminary, researchers theorize that it, “may protect cardiac myocytes by eliminating damaged organelles, such as mitochondria and protein aggregates, which would otherwise cause increases in oxidative stress and cellular dysfunction.”5
Intermittent fasting research also shows that autophagy may provide protection against other diseases, too, including neurodegenerative diseases like Alzheimer’s, and may be effective against cancer on its own, or as an enhancement of existing therapies. [26] [27]
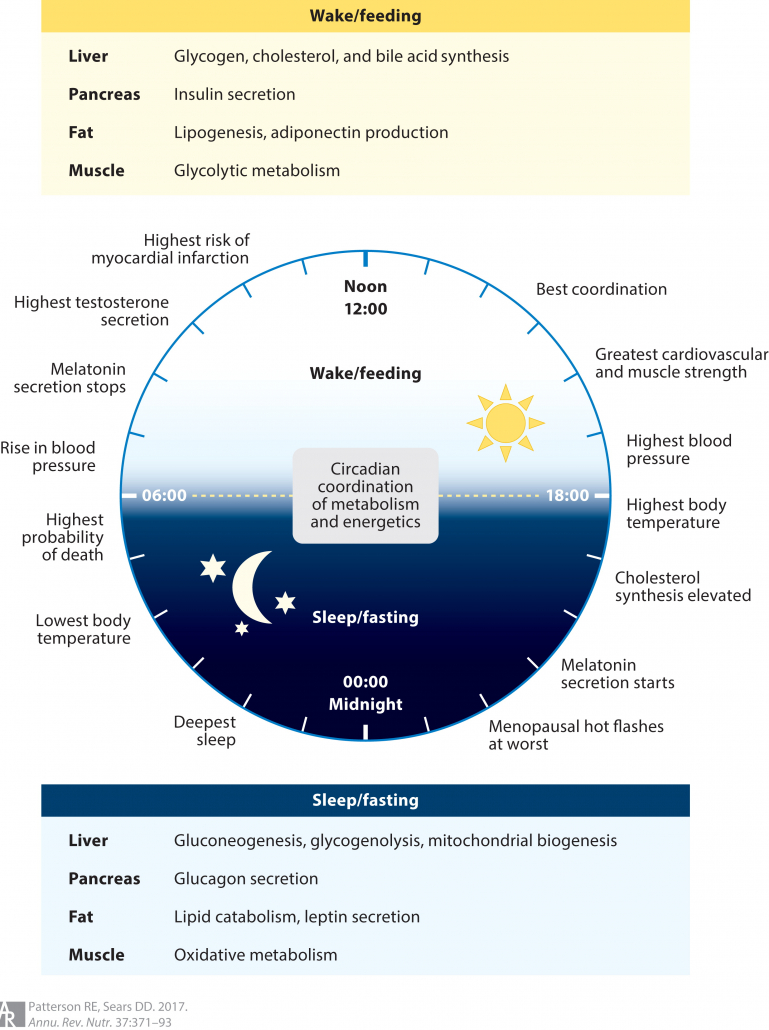
Circadian Rhythm Fasting
Intermittent fasting research has revealed that different time restricted fast regimens show widely varying results.
One of the most promising and effective strategies is called circadian rhythm fasting. This entails timing your meals to align with your body’s internal clock. It’s based on the idea that our metabolism works differently during each phase of the day.
Research looking specifically at the relationship between circadian rhythm, eating, and heart health have found that:
- Eating dinner late in the evening is associated with higher postprandial glucose levels than daytime meals, increasing the risk of diabetes.
- Misaligning eating with your circadian rhythm increases insulin resistance after only 3 days.10
- Eating at night decreases both quality and quantity of sleep. This exacerbates insulin resistance, obesity, and cardiovascular disease. 12,13.
- In studies, people who were allowed to eat during the middle of the day showed superior weight loss, less fat, greater glucose control, healthier lipid levels and reduced inflammation.14
- In contrast, subjects of intermittent fasting studies who were allowed to eat after 16:00 showed no improvement and even worsening of lipid levels, glucose control, and blood pressure. 15,16
Improved Mindfulness
Modern life offers many benefits and conveniences, but it also means being tempted by near-constant access to cheap, addictive, essentially poisonous foods.
Many people turn to these hyper caloric processed ‘foods’ in times of stress. Yet all this processed junk actually causes stress levels to rise, increasing insulin resistance, hypothyroidism, and nutrient deficiencies over time. [27]
Intermittent fasting can help. A 2020 study published in the Journal of Addiction Research found that fasting can retrain your brain and take the emotionalism out of eating.
Researchers stated, “Most if not all organ systems respond to intermittent fasting in ways that enable the organism to tolerate or overcome [food addiction]” [28]
For best results, of course, it’s also important to break your fast with nourishing, non-addictive foods. Highly satiating, animal-based superfoods can help!
For more support with food addiction, learn more about mindful eating here.
Intermittent Fasting Research: Takeaway
The intermittent fasting research is clear: Fasting works by activating various mechanisms to provide at least six different types of benefits:
- Hormone optimization
- Improved body composition
- Increased insulin sensitivity
- Reduced inflammation
- Improved heart health
- Improved mindfulness
Many people on IF say they feel better, think faster, and even look better than they have in years.
While more research is needed to fully elucidate all of intermittent fasting’s health benefits, the totality of research paints a supportive and encouraging picture for people practicing or thinking of practicing intermittent fasting.