We include products in articles we think are useful for our readers. If you buy products or services through links on our website, we may earn a small commission.
Keto and COVID-19: Boost Immunity and Reduce Risks

Table of Contents
Exciting results from a recent study show a ketogenic (keto) diet may be useful in mitigating the severity of COVID-19.
In this article, we’ll explore the link between metabolic health and risk of severe illness. And we’ll take a deeper look at the science behind the possible benefits of keto for COVID-19.
Diet and Immunity
Let’s start with a caveat: There’s no diet that will prevent a SARS-CoV-2 infection, the virus responsible for the COVID-19 global pandemic.
So it makes sense that throughout the pandemic, health agencies have focused their attention on vaccines, pharmaceuticals, and public health measures like wearing masks and social distancing.
Yet, as the age-old saying goes, you are what you eat. Most Americans eat a diet full of sugar and processed foods. And junk food leads to a junky immune system.
A 2014 review of numerous studies looking at the effects of the American diet on immunity found that, “our over abundance of calories, and the macronutrients that compose our diet may all lead to increased inflammation, reduced control of infection, increased rates of cancer, and increased risk for allergic and auto-inflammatory disease.”
The authors concluded that because of the dramatic impact that the food we eat has on our immunity, the link between diet and immunity should be given as much attention as is given to how diet impacts cardiovascular health.
Since no health issue has had nearly as large an impact on dietary guidelines as cardiovascular health, this is saying a lot!
The Link Between Metabolic Health and Severe Cases of COVID-19
Metabolism refers to all the chemical processes in your body necessary to maintain life. Energy production? Yes. Growth? Yup. Tissue repair? Of course. Fighting disease? Absolutely.
It should come as no surprise that poor metabolic health can have devastating consequences on your body.
Unfortunately, optimal metabolic health among American adults is shockingly low. In a recent National Health and Nutrition Examination Survey, only 12% of Americans are metabolically fit.
Although there is no strong consensus on an exact definition of “metabolic health,” it can be defined as the absence of metabolic syndrome.
A person with metabolic syndrome meets 3 or more of the following measurements:
- Waist circumference above 40 inches in men, 35 inches in women
- Systolic blood pressure (top number) above 120 mmHg, diastolic blood pressure (bottom number) above 80 mmHg
- Fasting glucose (blood sugar) level of 100 mg/dL or greater and HbA1c greater than 5.7%
- Triglyceride level of 150 mg/dL or greater
- High-density lipoprotein (HDL) cholesterol (the “good” cholesterol) less than 40 mg/dL in men, 50 mg/dL in women
Poor metabolic health puts you at a higher risk for many diseases, including:
- Coronary heart disease
- Stroke
- Type 2 diabetes
- Non-alcoholic fatty liver disease
- Cancer
- Polycystic ovarian syndrome
- Dementia
Source: American Institute for Cancer Research (https://www.aicr.org/resources/blog/healthtalk-a-healthy-weight-metabolic-syndrome-and-cancer-risk/)
Keto for COVID-19?
The keto diet has been a buzzword in the mainstream health and wellness field for the last few years.
By restricting carbs, and adding in high amounts of fat, the keto diet switches the body from using carbs for fuel, to a metabolic state called ketosis. In ketosis, your body uses fat as its primary fuel source.
Though keto receives a lot of attention for its association with rapid weight loss, there’s a lot more to it. In fact, it has been used therapeutically for decades as a treatment for epilepsy, metabolic disorders, heart disease, cancer, neurodegenerative diseases, diabetes, migraines, and many other conditions.
And now, medical experts are exploring how a keto diet can help prevent what they believe is the underlying cause of severe manifestations of COVID-19: cytokine storms.
What are Cytokines?
The phrase “cytokine storm” has captured the public spotlight since the start of the pandemic. Before delving into how cytokine storms are thought to impact the severity of COVID-19, it’s worth looking at what cytokines are.
Put simply, cytokines are a diverse group of small signaling molecules secreted by cells in a complex, coordinated response to bacteria, viruses, or other microorganisms that can cause disease.
Think of the immune system as an orchestra. The first immune cell (the conductor) to notice an invader sends out cytokines with a message that an immune response should be occurring. The cytokines carry the directions to other cells and organs (players), activating immune cells and producing more cytokines.
Inflammation is one type of immune response elicited by cytokines.
During acute inflammation, cytokines signal cell walls and blood vessels to become more permeable. Normally, only water and small molecules are permitted to exit the bloodstream into tissues. However, during inflammation, leaky blood vessels allow for a rapid influx of larger proteins and immune cells to the infected or damaged tissue.
Common symptoms of inflammation include:
- Fever
- Aches
- Heat
- Chills
- Fatigue
Once the infection is resolved, the immune response cools off and the dilated blood vessels return to their normal state.
Cytokine Storm
Cytokines are necessary and good for a healthy immune response. But sometimes they can be too much of a good thing.
In any immune response, pro-and anti-inflammatory cytokines are released simultaneously, and their balance is critical in maintaining lung homeostasis.
When this balance is disturbed or when the wrong type of cytokines is secreted early on in the immune response, a cytokine storm occurs.
Like a security alarm that doesn’t turn off even after law enforcement arrives, cytokines in a cytokine storm continue sounding the alarm. Since many cells throughout the body have cytokine receptors, the negative effects of a cytokine storm are systemic.
A direct correlation exists between cytokine storms and widespread tissue damage and poor prognosis of viral infections.
Acute lung injury or its more severe form, acute respiratory distress syndrome, are common consequences of a cytokine storm.
Intense inflammation in the lungs can spill over, leading to systemic effects. Patients experiencing cytokine storms suffer from reduced oxygen in the blood, difficulty breathing, and fluid build-up in the lungs. All these symptoms are seen with COVID-19.
Septic shock and multiorgan failure can also follow a cytokine storm and represent the main causes of mortality in severe COVID-19 cases.
Cytokine Storms and Metabolic Health
Little is known about the exact cause of the uncontrolled increase in cytokine release. But some researchers believe there are clues in glucose metabolism.
Early on in the pandemic, researchers were able to identify several risk factors that dramatically increased the risk of severe illness and death from COVID-19:
- Overweight or obesity
- Type 2 diabetes
- High blood sugar
- High blood pressure
This suggests a link between the pathogenesis of COVID-19 and the regulation of the host’s metabolism.
Viruses alter the host cells’ metabolism to optimize conditions for their rapid and efficient replication. In an influenza virus study, researchers identified a specific glucose metabolism pathway responsible for producing proinflammatory cytokines. They also found a strong correlation between blood glucose and cytokine levels.
SARS-CoV-2 also appears to favor a high glucose environment.
Upon infection by SARS-CoV-2, immune cells like macrophages and monocytes accumulate in the lungs.
The virus infects and re-programs monocytes to produce more angiotensin-converting enzyme 2 (ACE2), a key protein used by the virus to enter cells. The infected monocytes also induce higher levels of several proinflammatory cytokines associated with cytokine storms.
High blood glucose levels make the infection and replication process much easier. In fact, glycolysis, the breakdown of glucose, is necessary for SARS-CoV-2 replication. One study showed glucose directly increased viral load and expression of ACE2 and proinflammatory cytokines. This finding is consistent with what we already know is true — individuals with high glucose levels are more susceptible to COVID-19.
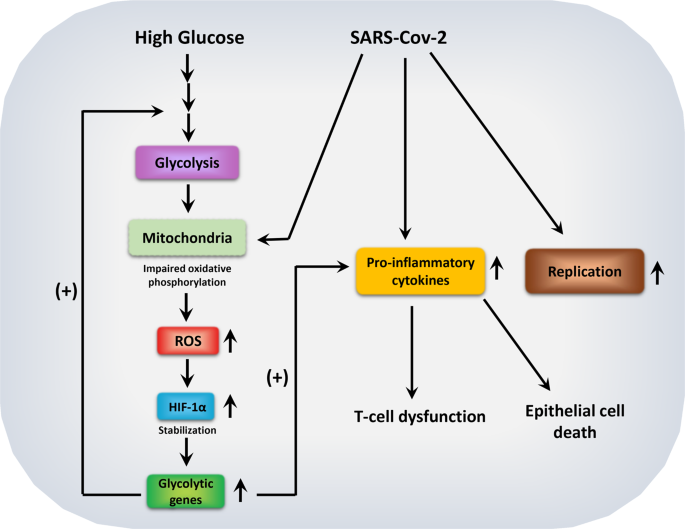
Image from nature.com
Increased glucose metabolism through aerobic glycolysis promotes replication of the COVID-19 virus and cytokine production. These factors compromise T-cell response and function. The end result is the death of lung cells.
Chronic low-grade inflammation is a common denominator of individuals with metabolic syndrome.
Abnormal glucose metabolism is also a hallmark of hyperglycemia and type 2 diabetes. With all of these factors combined, SAR-CoV-2’s entry and replication are enhanced, and the immune response is greatly exaggerated.
The bottom line? To minimize your risk of severe COVID-19, it’s time to get your metabolic health under control.
Keto and COVID-19: What Does Science Say?
It’s clear that dietary interventions are important to reduce the availability of glucose and mitigate the risk of a cytokine storm. Foods that raise glucose levels — and consequently increase inflammation — need to be substituted with those that have anti-inflammatory properties.
Enter the keto diet.
The five main components of metabolic syndrome are all improved by carbohydrate restriction. By limiting carbohydrates, insulin secretion can be stabilized and the fat stored in fatty tissue becomes liberated. The fatty acids then undergo a process called beta-oxidation in the liver’s mitochondria, producing acetyl coenzyme A (acetyl CoA) which generates ketone bodies.
The ketone bodies generated don’t just provide fuel for energy. They also protect against oxidative stress, increase antioxidants, and scavenge free radicals. Additionally, one ketone body in particular, beta-hydroxybutyrate (BHB), has been shown to regulate metabolism.
A large body of evidence lends support for the efficacy of the keto diet on blood glucose control. Because the keto diet promotes weight loss and prevents blood sugar spikes, patients with diabetes can gain better glycemic control and even regain insulin sensitivity.
What About a Low Fat Diet?
You might be thinking: why not just eat a low-fat diet? Wouldn’t that help with weight loss and metabolic syndrome?
Not so fast.
Despite popular belief, eating healthy fats is one of the best things you can do to protect against inflammation.
In one study, researchers compared a keto diet with a low-fat diet in 40 subjects with high levels of cholesterol in their blood. While both diets improved several metabolic markers, only the subjects on the keto diet had consistent reductions. The keto diet also showed favorable changes in other indicators of heart disease risk and in proteins linked to insulin resistance.
Want to learn more about the keto diet? Read our in-depth guide here.
Boosting Your Immune System with Vitamins and Minerals
So what are some foods that boost your immune system, especially during COVID-19?
Nutrients are most potent when they come from fresh, whole foods. Let’s take a look at some of the most common under-consumed vitamins and minerals, and where they can be found in a keto diet.
- Vitamin C can increase the production of B-lymphocytes, which are then able to produce more antibodies. Some citrus fruits, red/green pepper, kiwi, broccoli, and strawberries are high in vitamin C.
- Vitamin D influences over 2,000 genes in our bodies. Sun exposure is the best way to get vitamin D, but it can also be found in cod liver oil, fish, mushrooms, fortified milk, and eggs.
- Vitamin A is known as an anti-inflammation vitamin. A powerhouse source of highly bio-available vitamin A include beef liver and chicken liver.
- Vitamin E is another compound with powerful antioxidant properties. Salmon roe, tuna fish, and green leafy vegetables are among the best keto-friendly sources of vitamin E.
- Zinc is critical for immune function and can be found in all body tissues. Oysters, red meat, and poultry have high zinc content.
- Selenium can enhance the immune system to decrease the risk of infection. Seafood, red meat and poultry, and organ meats are great food sources of selenium.
- Magnesium is involved in over 300 enzyme reactions in the human body, including those that support the immune system. On a keto diet, it can be found in seafood including mackerel, sardines, salmon, sea bream and halibut, in green leafy vegetables, bone broth, and avocados.
- Omega-3 fatty acids aren’t just good for your skin and hair; they can also exert antiviral effects. Some believe they can improve oxygenation in patients with COVID-19. Salmon, oysters, and sardines are rich sources of omega-3 fatty acids.
Keto and COVID-19: The Outlook
Obesity, high blood pressure, high blood sugar, and diabetes are all associated with metabolic syndrome. You might think that as long you’re not overweight, you’re in good shape metabolically.
But metabolic health is not just about weight — metabolic syndrome can affect anyone.
Studies have pointed to metabolic syndrome as the underlying cause of many diseases. And now, some experts think that treating metabolic syndrome may be the key to fighting COVID-19. And the keto diet can help.
Though no diet will offer 100% protection against COVID-19, changes to our diet can dramatically reduce many risk factors.
When considering the evidence, a nutrient-rich keto diet reduces the potential for a cytokine storm as a result of an infection from COVID-19, or any virus for that matter.