We include products in articles we think are useful for our readers. If you buy products or services through links on our website, we may earn a small commission.
Histamine Intolerance: Everything You Need to Know
Table of Contents
- Histamine Fast Facts
- Histamine Basics
- What is histamine intolerance?
- Symptoms of histamine intolerance
- What causes histamine intolerance?
- How to diagnose histamine intolerance
- Histamine intoxication vs. histamine intolerance
- Symptoms of histamine intoxication
- How to reduce histamine in the body
- Low histamine diet tips
- Other ways to reduce histamine intolerance
- Histamine intolerance is treatable
Did you know that the allergy symptoms you experience may not be due to allergies at all? They may be a common condition called histamine intolerance.
Histamine intolerance occurs when your body lacks the ability to process excess histamine and reacts negatively to the buildup that occurs.
In this article we will discuss what histamine is, the causes of histamine intolerance, and also provide helpful tips for how to eliminate the effects of histamine intolerance by introducing a low histamine diet along with other helpful tips.
Histamine Fast Facts
- Histamine is an essential part of a healthy immune system.
- Histamine is released after injury or when an invader is detected.
- When your body releases histamine it recruits other important immune cells to the site to deal with the injury or invader.
- Excess histamine that causes histamine intolerance is often absorbed through our gut from the food we eat or microorganisms living symbiotically in our intestines.
- Our body normally has enzymes in the gut that break down histamine.
- The production of these enzymes cab be affected by genetics, and medications that prevent our body from breaking down histamine in the gut.
- When these enzymes are inhibited, high levels of histamine can build up in the bloodstream, and you are susceptible to histamine sensitivity.
- Common symptoms of histamine intolerance include, bloating, headaches, and rashes, among many others.
- There are several ways to reduce histamine intolerance including diet, supplements, and medications.
Histamine Basics
Histamine is produced and stored by cells in your immune system. White blood cells called mast cells and basophils are the primary producers of histamine. But many other immune cells are also involved.
When the immune system identifies foreign invaders, your immune cells release histamine. Histamine then triggers an immediate inflammatory response. This sends immune cells to the source of infection, which allows them to destroy the pathogens and fight infection.
Sometimes, your immune system mistakenly identifies harmless substances like certain foods or pollen as foreign invaders. This process of mistaken identity results in an allergic reaction.
In addition to playing an important role in the immune response, histamines regulate many other physiological functions in the body by:
- Secreting gastric acid
- Dilating blood vessels
- Contracting and relaxing the airways and other smooth muscles
- Transmitting messages between your body and brain
- Increasing vascular permeability
- Lowering blood pressure
- Producing airway mucus
- Regulating energy levels
- Enhancing cognition
Histamine Metabolism
Histamine metabolism occurs when histamine is released in the body and is eventually captured by receptors and broken down. This process is an essential part of a healthy immune system.
When invasive compounds like pollen enter your body, histamine leaves your mast cells and flows to the affected area. This causes inflammation, which allows other immune cells to go to work fighting infection. Histamines then connect with receptors in your body where it’s eventually broken down and expelled as waste. This prevents chronic inflammation and allows your body to return to a normal, healthy state.
Your body metabolizes histamine through two pathways using the enzymes DAO, and HNMT.
Diamine oxidase (DAO)
When you ingest histamine with food DOA acts like a scavenger, finding and breaking down histamine. It also scavenges histamine that your intestinal microorganisms produce. This prevents histamine from being absorbed into the bloodstream from the gastrointestinal tract.
The DAO enzyme accumulates in the following tissues:
- Small intestine
- Large intestine
- Placenta
- Kidneys
Histamine-N-methyltransferase (HNMT)
HNMT also prevents the absorption of dietary histamine, and breaks down histamine that has made its way into the blood.
HNMT is present in many areas of the body including:
- Kidneys
- Liver
- Spleen
- Large intestine
- Prostate
- Ovaries
- Spinal cord
- Trachea
- Respiratory tract
What is histamine intolerance?
Histamine intolerance is a disorder that occurs as a result of an inability to metabolize dietary histamine. This is due to reduced DAO enzyme activity, which leads to an accumulation of histamine in the bloodstream. Histamine intolerance is not an allergy. Rather, it’s an intolerance to the chemical histamine.
Histamine intolerance is also known as:
- Enteral histaminosis
- Sensitivity to dietary histamine
Symptoms of histamine intolerance
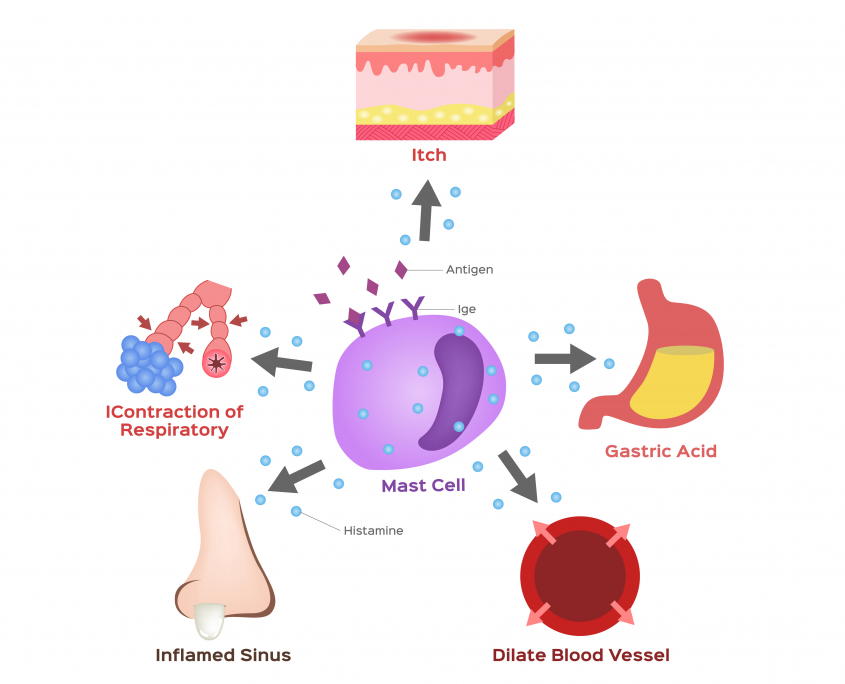
Histamine intolerance often causes a combination of symptoms that range from mild to severe. In some cases, histamine intolerance can even result in death.
Histamine intolerance can present as symptoms that affect your entire body including, your gastrointestinal, nervous, cardiovascular, respiratory, and integumentary systems.
Symptoms of histamine intolerance may include:
- Abdominal distension
- Bloating
- Postprandial fullness
- Diarrhea
- Abdominal pain
- Constipation
- Dizziness
- Fatigue
- Headaches
- Palpitations
- Hay fever
- Conjunctivitis
- Pruritus
- Hives
- Eczema
- Erythema
- Edema
- Asthma
- Hypoxia
- Anaphylaxis
Generally, the greater the buildup of histamine in the body the more severe the symptoms.
What causes histamine intolerance?
Many factors may lead to the development of histamine intolerance. We’ll explore these factors below.
Genetics
Your genetics can influence your ability to break down histamine.
More than 50 DNA sequence variations exist that may inhibit histamine metabolism. Additionally, some genes can cause mutations in the DAO enzyme that reduce its ability to metabolize histamine.
Disease
Inflammatory bowel conditions may impair DAO activity by damaging intestinal mucosal integrity. These conditions include:
- Gastroenteritis
- Irritable bowel syndrome (IBS)
- Inflammatory bowel disease (IBD)
- Short bowel syndrome
- Gastrointestinal surgery
People with nonceliac gluten sensitivity (NCGS) may also have an increased risk of reduced DAO enzyme activity.
Medication
Certain medications may reduce the activity of the enzyme DAO.
The following medications may block DAO:
- Chloroquine (antimalarial)
- Clavulanic acid (antibiotic)
- Verapamil (antihypertensive)
- Cimetidine (antihistamine)
- Colistimethate (antibiotic)
- Cefuroxime (antibiotic)
- Clonidine (antihypertensive)
- Dihydralazine (antihypertensive)
- Pentamidine (antiprotozoal)
- Isoniazid (antituberculosis)
- Metamizole (analgesic)
- Diclofenac (analgesic and anti-inflammatory)
- Acetylcysteine (mucoactive)
- Amitriptyline (antidepressant)
- Metoclopramide (antiemetic)
- Suxamethonium (muscle relaxant)
- Prometazina (antihistamine)
- Ascorbic acid (vitamin C)
- Thiamine (vitamin B1)
How to diagnose histamine intolerance
Histamine intolerance can be hard to diagnose because the symptoms are nonspecific and are similar to many allergic reactions. Moreover, there are few validated diagnostic tools to confirm a histamine intolerance diagnosis.
Unfortunately, many people with histamine intolerance end up visiting several doctors before receiving an accurate diagnosis. And many people may go undiagnosed.
The diagnostic criteria for histamine intolerance include:
- Typical symptoms associated with histamine intolerance
- Exclusion of other disorders
The following methods can rule out other potential causes of elevated histamine levels:
- Skin allergy test
- Tryptase blood test
- Review of medications
If the above methods rule out other conditions such as a food allergy or mastocytosis, a diagnosis of histamine intolerance is confirmed if you have two or more typical symptoms that improve after a low histamine diet.
Histamine intoxication vs. histamine intolerance
Histamine intoxication is a form of food poisoning that occurs with excessive histamine ingestion. This condition is entirely separate from histamine intolerance. Histamine intoxication can occur in healthy people after consuming high histamine foods such as:
- Spoiled fish or meat
- Fermented foods
High levels of histamine can form in spoiled or fermented foods when live bacteria produce histamine. Excessive levels of histamine can overpower the DAO enzyme, which results in histamine intoxication.
Histamine intoxication is also known as:
- Scombroid fish poisoning
- Mahi-mahi flush
- Scombrotoxicosis
- Histamine poisoning
- Histamine toxicity
Symptoms of histamine intoxication
Histamine intoxication can cause symptoms that are similar to those of histamine intolerance. These usually occur within one hour of ingesting food and are usually mild to moderate in severity. After a few hours, the symptoms generally resolve on their own.
Symptoms of histamine intoxication may include:
- Skin redness
- Rash
- Hives
- Edema
- Nausea
- Vomiting
- Diarrhea
- Low blood pressure
- Headache
- Palpitations
- Numbness and tingling
How to reduce histamine in the body
Understanding how to reduce histamine in the body is essential for individuals with histamine intolerance. Treatment for histamine intolerance focuses on decreasing the buildup of histamine levels. Below, we’ll discuss the best strategies to reduce histamine in the body.
Low histamine diet
Many foods naturally contain histamine. Consuming a low histamine diet can improve symptoms of histamine intolerance in 4 to 8 weeks by reducing histamine levels in the body.
A low histamine diet is a temporary plan that involves consuming foods that contain histamine levels below detection limits.
An important note: Though low histamine foods include certain fruits and plants, it is possible to confuse histamine intolerance with chronic low-grade food allergies. Plants are packed with numerous naturally occurring plant toxins. That’s why we strongly recommend animal and dairy based diet to reduce diet-related disorders and inflammation.
Low histamine foods that are safe to eat on a low histamine diet include:
- Fresh meat
- Fresh fish
- Fresh fruits
- Vegetables
- Green pepper
- Peas
- Asparagus
- Cauliflower
- Beans
- Eggs
- Olive oil
- Non-dairy milk
- Coconut milk
- Whole grains
- Oats
- Rice
- Barley
Some foods that are low in histamine can be high in other biogenic amines that result in histamine intolerance. These reactions occur because the enzyme DAO also metabolizes biogenic amines including:
- Putrescine
- Cadaverine
- Tyramine
Foods that contain high levels of biogenic amines may occupy DAO and reduce the metabolism of histamine.
The following low-histamine foods are high in biogenic amines:
- Soybeans
- Mushrooms
- Lentils
- Chickpeas
- Peanuts
- Pears
- Citrus fruits
- Bananas
Many people with histamine intolerance may need to eliminate foods high in both histamines and biogenic amines. But others may not experience any symptoms when eating these foods.
While following a low histamine diet, eliminate high histamine foods.
Foods high in histamine include:
- Spoiled fish or meat
- Fermented foods
- Yogurt
- Cheese
- Kombucha
- Sauerkraut
- Vegetables
- Spinach
- Avocados
- Tomatoes
- Eggplant
- Dried fruit or fruit juices
- Alcohol
- Beer
- Wine
- Champagne
Your symptoms should resolve within 3 weeks of starting a low histamine diet. After this, you can then begin adding higher histamine foods back into your diet one by one.
If any of these foods trigger symptoms of histamine intolerance, you should continue to avoid them. But it is possible to safely consume high histamine foods that don’t bother you.
Low histamine diet tips
Maintaining a low histamine diet can improve your health and prevent complications related to histamine intolerance. But this diet plan is only a temporary treatment and can result in malnutrition.
To reduce histamines while providing your body the macro and micronutrients it needs to thrive, we recommend high fat low carb eating. Diets like paleo, keto, and carnivore all great options.
Some tips to successfully follow a low histamine diet include:
- Always eat fresh foods. Histamine and other biogenic amines may form during refrigerated storage. Spoiled foods can grow bacteria that produce histamine.
- Boil vegetables in water before eating. This can reduce the levels of histamine and other biogenic amines in food.
- Keep a food journal to identify trigger foods. A food journal can help you determine what foods cause your symptoms. Keep track of the foods you eat, what time you eat them, and any uncomfortable symptoms that you experience.
- Work with a dietician or nutritionist. A low histamine diet is restrictive. You should not follow this diet plan for more than 4 to 8 weeks. Working with a dietician or nutritionist during a low histamine diet can ensure you receive the proper nutrients you need. We recommend finding a professional well-versed in low-carb high-fat eating.
- Avoid processed foods. Processed foods typically contain long lists of complex ingredients. Stay away from anything with trans-fats.
- Cook your own meals. You’ll know exactly what you’re eating.
- Avoid DAO blocking medications. Certain medications can slow down the healing process by impairing your ability to metabolize histamine.
- Take a DAO supplement. Increasing the enzyme DAO can reduce histamine in the body.
- Slowly reintroduce histamine-rich foods. A low histamine diet is only temporary. After you eliminate histamine-rich foods for 3 weeks, you can begin adding some foods back into your diet. Begin with full-fat dairy since it contains essential fat soluble vitamins A and D.
- If certain foods reproduce your symptoms, cut them out. But enjoy histamine-rich foods that don’t cause any problems.
Other ways to reduce histamine intolerance
Diamine oxidase supplement
Histamine intolerance occurs with elevated histamine levels, which is likely due to an impaired ability of diamine oxidase to metabolize histamine.
Fortunately, research shows that oral diamine oxidase supplements before meals can improve over 22 symptoms of histamine intolerance. Diamine oxidase oral supplements may improve symptoms of histamine intolerance by increasing diamine oxidase levels, which facilitates the breakdown of histamine.
However, diamine oxidase supplements are not a cure for histamine intolerance. Without diamine oxidase supplementation, symptom intensity increases.
Antihistamines
Antihistamines like Zyrtec, Allegra, and Benadryl are popular choices for the treatment of allergies. But can these medications also help with histamine intolerance?
The answer is yes. But only to a certain degree. Taking antihistamines will not reduce histamine in the body. Antihistamines only treat symptoms that you experience after ingesting foods high in histamine.
Avoid the following antihistamines that reduce the efficacy of DAO:
- Cimetidine
- Prometazina
Many antihistamines can cause side effects such as:
- Drowsiness
- Dizziness
- Constipation
- Dry mouth
- Blurred vision
- Headache
Histamine intolerance is treatable
Histamine regulates many important physiological functions in the body, but it can also cause negative consequences like histamine intolerance.
The best way to combat histamine intolerance is to follow a low histamine diet. High fat, low carb animal-based diets will allow you to cut out histamine rich foods while still providing your macro and micro nutrient needs.
Proper food preparation is also key to prevent increasing levels of histamine.
If you regularly experience symptoms of histamine intolerance even after practicing a low histamine diet, we recommend going a step further and cutting out most plant foods. This will reduce your exposure to plant toxins.
Histamine intolerance often occurs in combination with underlying intestinal disorders, and symptoms may not resolve unless you treat both. With a dedicated treatment plan, you can find long-term relief from histamine intolerance.
















